Us covid deaths by race9/16/2023  When you have poor educational outcomes, you have limited employment opportunities. If you have a poor neighborhood, then you’ll have poorly funded schools, which often results in poor education outcomes and another generation lost. (Nothing differential by race just so happens.) It is tied to residential and educational segregation in this country. The overrepresentation in these jobs doesn’t just so happen. And those frontline jobs-which, for a long time, have been invisibilized and undervalued in terms of the pay-are now categorized as essential work. 
We are more exposed because of the kinds of jobs that we have: the frontline jobs of home health aides, postal workers, warehouse workers, meat packers, hospital orderlies. Why do you say Black, brown and Indigenous people are more exposed? Then, once infected, we are more likely to die because we carry a greater burden of chronic diseases from living in disinvested communities with poor food options poisoned air and because we have less access to health care. It does so through two mechanisms: People of color are more infected because we are more exposed and less protected. She is currently a Presidential Visiting Fellow at the Yale School of Medicine and is writing a book proposing strategies for a national campaign against racism.Īs the country began to confront the unequal impact of COVID and the ongoing legacy of racial injustice it represents, Jones spoke with Scientific American contributing editor Claudia Wallis about the ways that discrimination has shaped the suffering produced by the pandemic.Īlong with age, male gender and certain chronic conditions, race has turned out to be a risk factor for a severe outcome from COVID. As president of the American Public Health Association in 2016, she led a campaign to explicitly name racism as a direct threat to public health. For 14 years Jones worked at the CDC as a medical officer and director of research on health inequities. Racism, she explains, has led people of color to be more exposed and less protected from the virus and has burdened them with chronic diseases. The reason for these disparities is not biological but is the result of the deep-rooted and pervasive impacts of racism, says epidemiologist and family physician Camara Phyllis Jones. Compared with non-Hispanic white people, American Indian, Black and Latinx individuals, respectively, faced 3.5, 2.8 and 3.0 times the risk of being hospitalized for the infection and 2.4, 1.9 and 2.3 times the chance of dying, according to the Centers for Disease Control and Prevention. The disease has disproportionately harmed and killed people of color. 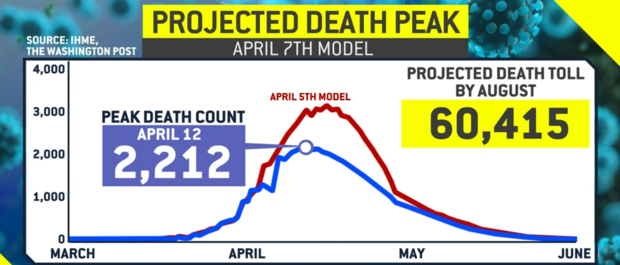
The article was published independently and without sponsorship.ĬOVID-19 has cut a jarring and unequal path across the U.S. 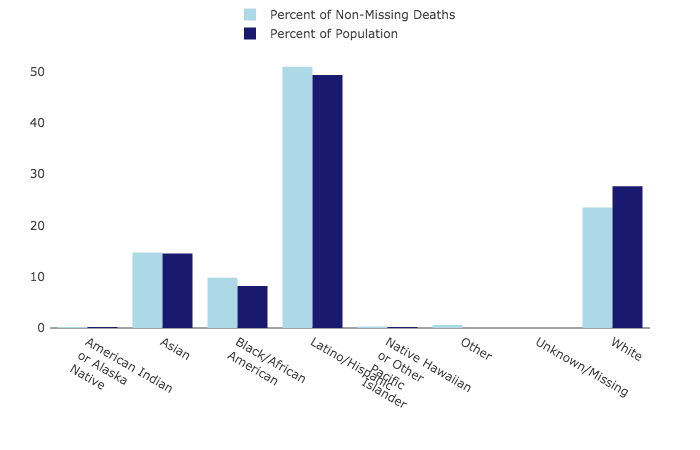
Editor’s Note (12/21/21): This article is being showcased in a special collection about equity in health care that was made possible by the support of Takeda Pharmaceuticals. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
